Revolutionising Acute Myocardial Infarct (AMI) at Bart’s Heart Centre
Summary
Ortus-iHealth revolutionises AMI follow-up at Barts Heart Centre.
Barts Heart Centre is one of the largest cardiac centres in Europe and globally recognised as delivering a highly effective, fast, and efficient service for over 80,000 patients per year who suffer a heart attack.
Barts Heart Centre has been using Ortus-iHealth since 2018. Since then, use of Ortus has expanded into a number of pathways including across cardiology and oncology. This case study explores the benefits and successes of Ortus-iHealth at Barts Heart Centre, for both patients and clinicians.
The Problems:
- Barts Health Centre lacked the capacity to follow-up with patients consistently
- Ensuring medication titration and compliance post-procedure is difficult
- Impact of COVID-19 on face-to-face appointments
- Inconsistent PROMs, PREMs and Vitals data
The Goals:
- Increase follow-up capacity with heart attack patients
- Improve medication titration and compliance post-procedure
- Increase efficiency with outpatient appointments and shorter waiting times
- Collect more patient data, monitoring and reporting PROMs, PREMs and Vitals
The Ortus Solution:
The team at Barts were able to address multiple factors that contributed to everyday challenges at the clinic. These included:
- Appointment management because of high volumes
- Clinical resource shortages
- Patient DNA and patient access issues
- Inconsistent and inefficient patient data collection
By modelling standardised care pathways digitally and providing patients and clinicians with a digital platform with which they could monitor patients and communicate, schedule appointment, manage consent and provide patient education and information with, both parties where able to experience more productive and convenient consultations, saving time and boosting productivity.
Some of the tools used included:
- Remote patient monitoring of both symptoms and vitals
- Biometric, Proms and Questionnaire collection
- Enabling of digital consent
- Proactive delivery of Patient Access to key information
- Virtual Wards and telehealth consultations
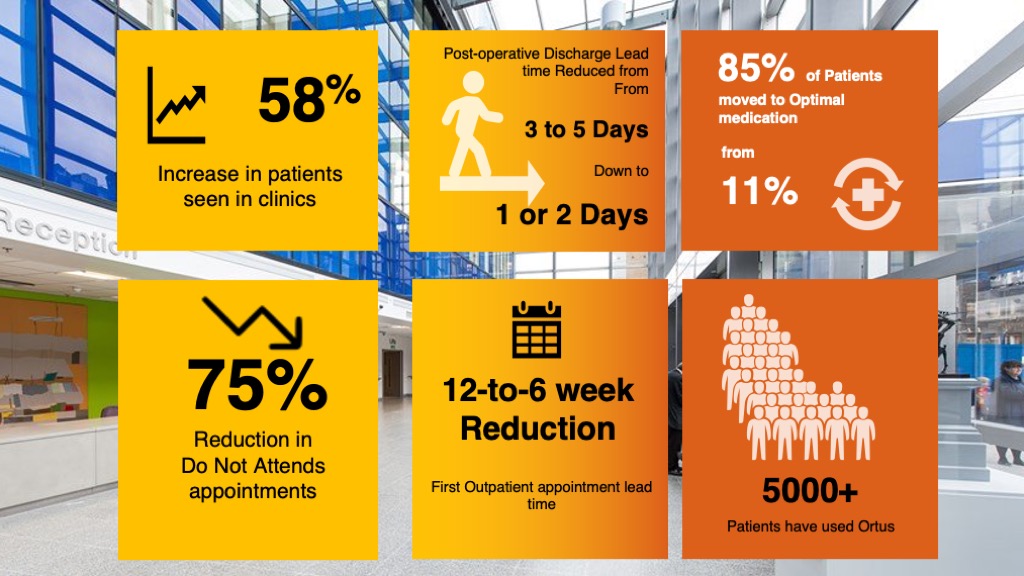
The Results
- Increase in patients seen in clinics
- Reduced post-operative discharge time
- Reduction in DNAs
- Increase in medicine titration and optimisation
- Savings in time and increased efficiency vs. face-to-face
- Designed and implemented a 24-hour discharge process during COVID-19
Results – Patients’ Feedback

Results – Clinicians’ Feedback
And on Medication
Prior to the remote monitoring only 11% of patients saw changes to their medication, after 88% of patients saw adjustments to the recommended dose.

